(5 Minute Read)
As emergency department utilization continues to steadily increase, health plans must strategically limit their cost exposure. Every year there are approximately 139 million visits to the emergency room in the USA (CDC), with up to 70% of them being for non-emergency causes. Whenever a new health scare emerges, the number of non-emergency visits jumps significantly, leading to an overuse of the system.A large portion of ER visits falls into the category of avoidable use resulting from patients seeking non-urgent care or ER care for conditions that could have been treated and/or prevented by primary care. Avoidable utilization of the ER diminishes the quality of care due to crowding, long waits, and added stress on staff- resulting in over 8 million dollars a year in unnecessary spending (Modern Healthcare).
Payer organizations struggling to achieve the triple aim of improved patient care and experiences while reducing costs may benefit from exploring ways to minimize the over-utilization of the emergency room services by their members. By proactively steering members toward a different action (visiting a clinic, contacting a help line before visiting, etc.), health plans can prevent the high claims costs associated with these often avoidable trips to the ER.
Below are 4 ways that payer organizations can help their members to get the care they need in the appropriate place...
IDENTIFY & TARGET YOUR SUPER-USERS
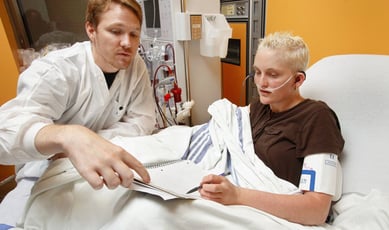 Organizations working to change their cost structure and improve outcomes must design interventions that target high-risk, high-cost patients who need to be carefully and proactively managed. Fewer than 1 percent of patients in the U.S. account for nearly 22 percent of health care spending, with an average expenditure of $90,000 per patient. A large percentage of these costs can be attributed to frequent, but often preventable visits to the emergency room and hospital admissions by a relatively small number of patients (Research in Action).
Organizations working to change their cost structure and improve outcomes must design interventions that target high-risk, high-cost patients who need to be carefully and proactively managed. Fewer than 1 percent of patients in the U.S. account for nearly 22 percent of health care spending, with an average expenditure of $90,000 per patient. A large percentage of these costs can be attributed to frequent, but often preventable visits to the emergency room and hospital admissions by a relatively small number of patients (Research in Action).
Given the complex medical and social needs of ER frequent users, case management has been extensively used in this group, with multiple studies showing a successful reduction in the use of ER services and the cost of care. One study found that the average number of yearly, per patient emergency department visits dropped from 26.5 to 6.5 following the implementation of a case management program (Pope).
Develop a strategy to identify patients who would most benefit from care management, using population segmentation/risk stratification algorithms. Care Management Platforms (Such as TCS Healthcare Technologies, Essette, MHK, or Zeomega ) can offer insight into who is over-utilizing the ER, as well as population data clusters showing areas of concern and improvement.
Generate a report of those who have been in the ER four or more times in the last 12 months and reach out to make your educational tools available to them. Assign a care manager or social worker to be a point person supporting those patients that need additional help.
Don't have a care management program? Impresiv Health can help you identify, evaluate, acquire, and implement a new care management program. Click HERE to learn more.
EDUCATE YOUR MEMBERS
Emergency department overuse commonly occurs because patients don’t understand where they should go for care. Providing patients with educational materials and empowering them to manage their conditions, where appropriate, is another way to reduce ED visits. Educate your members by launching a marketing campaign aimed at directing them towards the appropriate provider type.
Communicate with your members repeatedly in many different forms to ensure success. Beyond educating them on their treatment options, including information such as the cost of visits and average wait times. Education empowers the patient to make an informed decision on where they will seek treatment.
Create marketing materials that show where patients can find urgent care facilities and retail clinics in their area, as well as what telemedicine options they have available to them. Create a list of common conditions, concerns, and injuries, with where members should go to receive care for each one.
Colorado’s “Where for Care” campaign is a collaborative effort of area healthcare organization that includes a website educating its citizens on where they should go for various concerns. There are pages also included helping patients understand their insurance coverage and how to contact their insurance carrier.
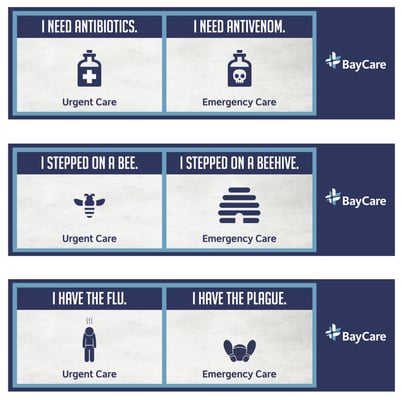
BayCare, one of the largest health care system in the Tampa Bay and West Central Florida area, took a humorous approach to minimizing ER over-utilization. They launched a series of easily understood billboards aimed at teaching Floridians where to go for care.
OFFER TELEMEDICINE AS AN ALTERNATIVE TO THE ER
Telemedicine has exploded into the healthcare space in recent years, with more and more Americans taking advantage of it. Telemedicine provides patients with access to immediate primary care consultations, proven to reduce emergency department overuse.
A recent analysis found that nearly 28% of all visits to a pediatric emergency department could have been handled with telemedicine (Kaiser). By enabling doctors to communicate with patients online, telemedicine can save time for both healthcare professionals and patients. This is especially true for injuries and illnesses requiring minimal exams. The Veterans Health Administration saved nearly $1 billion in 2012 after implementing telemedicine and other mobile health services (CMS).
To combat over-utilization of the ER, offer members the option of seeing a telemedicine provider. Promoting the 24/7 access to a physician from the comfort of home, after hours, is an effective way to minimize ER visits for non-emergency needs.
Unfortunately, convincing people to adopt a new way of receiving healthcare can come with challenges, and virtual care is no exception. One of the most effective ways to drive customers to virtual channels is awareness and education. Once again, you'll need to develop a campaign to help your members understand their options for care. Disseminate materials to your members explaining in multiple ways in multiple media about the telemedicine option, as well as information about what is appropriate for a telemedicine visit.
CONNECT VULNERABLE PATIENTS TO APPROPRIATE SERVICES
 Despite its purpose as a safety net for patients needing emergency stabilization, the ER is increasingly being used to combat access barriers. Emergency departments are the only place in the U.S. health care system where individuals have access to a full range of services at any time regardless of their ability to pay or the severity of their condition. Today, the ER is becoming a primary resource for more and more people as the primary care system finds itself unable to meet the growing demand for care.
Despite its purpose as a safety net for patients needing emergency stabilization, the ER is increasingly being used to combat access barriers. Emergency departments are the only place in the U.S. health care system where individuals have access to a full range of services at any time regardless of their ability to pay or the severity of their condition. Today, the ER is becoming a primary resource for more and more people as the primary care system finds itself unable to meet the growing demand for care.
Frequent emergency department users often seek care there as a result of mental health needs or substance abuse problems. A study by the Kaiser Family Foundation found that 18% of frequent ER users (defined as a patient who used the ER four or more times in the two-year study period) had a mental health condition compared to only 6% of the total study population. As emergency facilities see a significant number of patients with substance abuse and mental health needs, linking patients with appropriate support services can reduce this over-utilization.
Another vulnerable population requiring attention are those with language barriers. The increasing diversity of the nation brings opportunities and challenges for health care providers, health care systems, and policymakers to create and deliver culturally competent services. Language and cultural beliefs play a vital role in the interaction between patients from diverse cultural groups and physicians. Patients with limited English proficiency are more likely to return to the ER unexpectedly and more likely to experience a medical error due to inaccurate translations (Reuters Health). To combat this trend, payer organizations are designing culturally tailored programs and materials to alleviate this social determinant of health.
Click HERE to Read Impresiv Health's Blog: Tackling SDOH One Question at a Time.
Learn More About Impresiv Health's Clinical Services
Learn More About Impresiv Health's Professional Services
Never Miss Another Impresiv Health Blog
Sign up for our monthly newsletter to get the latest news, blogs, tips, and thought leadership from Impresiv Health.
References
Bhatnagar, Anupam, and Kishore Bharatula. Preventing Unnecessary Emergency Room Visits to Reduce Health Care Costs. Fractal Analytics, fractal.ai/wp-content/uploads/2018/06/Preventing-unnecessary-emergency-room-visits-to-reduce-health-care-costs.pdf.
Doyle, Kathryn. “Return Visits to the ER More Likely for Patients with Limited English.” Reuters, Thomson Reuters, 30 Apr. 2016, www.reuters.com/article/us-health-quality-emergency-language/return-visits-to-the-er-more-likely-for-patients-with-limited-english-iduskcn0xp2qo.
“faststats - Emergency Department Visits.” Centers for Disease Control and Prevention, Centers for Disease Control and Prevention, 19 Jan. 2017, www.cdc.gov/nchs/fastats/emergency-department.htm.
Kaiser Family Foundation. “Characteristics of Frequent Emergency Department Users.” The Henry J. Kaiser Family Foundation, 30 Sept. 2007, www.kff.org/health-costs/report/characteristics-of-frequent-emergency-department-users/.
Pope, D, Fernandes, CMB, Bouthillette, F, Etherington, J. Frequent users of the emergency department: a program to improve care and reduce visits. CMAJ 2000;162(7):1017-20
The High Concentration of U.S. Health Care Expenditures, Research in Action, Issue 19 Agency for Healthcare Research and Quality
Weiss A, Schechter M, Chang G. Case management for frequent emergency department users. Psychiatric Serv. 2013;64(7):715–6.









